{If you missed Part I you can read it here.}
First, before I started writing this post I never really realized that we have no photos from my hospital stay - probably cause we were a little busy and I looked like crap! But it would have been nice to have had something from this time period. Come to think of it, Matt and I don't have a photo of us together with Greta from any of our hospital/NICU stay...I was always taking the photos and I guess we never thought to ask family or the nurses to capture one of us together. It's unfortunate but we had so much more on our minds at this time. I really wish that I would think to capture moments on camera more often.
Anyways, on to the rest of the birth story (hunker down with a coffee it's long - I don't blame you if you skim it):
First, before I started writing this post I never really realized that we have no photos from my hospital stay - probably cause we were a little busy and I looked like crap! But it would have been nice to have had something from this time period. Come to think of it, Matt and I don't have a photo of us together with Greta from any of our hospital/NICU stay...I was always taking the photos and I guess we never thought to ask family or the nurses to capture one of us together. It's unfortunate but we had so much more on our minds at this time. I really wish that I would think to capture moments on camera more often.
Anyways, on to the rest of the birth story (hunker down with a coffee it's long - I don't blame you if you skim it):
It was around 10 am on Monday, I was still sitting in triage with the fetal monitor around my belly when the intern and resident came to deliver the news. My bloodwork had come back and it showed highly elevated liver enzymes and a very low platelet count, confirming that as suspected it was HELLP syndrome. The young female resident (who I must say was great!) began to explain to us what the next course of action and events would entail. First, the syndrome was again explained to us fully - highlighting that the cause of why it occurs is not exactly known, but they believe that the body began to reject the placenta for any number of reasons. Next, I would undergo a fetal assessment in order to ensure the baby was healthy and to check there was adequate blood flow from placenta to baby. The results of the fetal assessment would then determine how quickly delivery would need to occur. Things could change from hour to hour OR minute to minute it all depended on what was happening with me. Lastly, it was explained how crucial it was that I receive a corticosteroid injection as it would help to reduce the risk of complications when the baby was delivered early as it would help to stimulate faster lung development. I received the injection within minutes and then we waited to be taken to the fetal assessment.
I believe I was offered a wheelchair when we were transported to the fetal assessment, but I declined and walked to the fetal assessment (while writing this I asked my husband why I walked, and he says that I was so determined that I was not that ill), I think I should have set my pride aside and just went in wheelchair but anyways - we walked. We had an awesome ultrasound technician for the fetal assessment - she explained everything she was doing, told us what she was measuring and assured us that the baby was looking great. I did not have very good experience with ultrasound techs earlier in my pregnancy as I found them very cold and would never talk or explain anything - I get they can't say much as they aren't doctors but I always felt weird after previous ultrasounds! Her compassion and reassurance was really what we needed at this point! Following the fetal assessment I was admitted to the Antepartum unit to be monitored for the next 24-48 hours.
For the rest of the afternoon we rested, prepared questions for the doctors who we would be meeting with and just tried to put into perspective what was going on. It had been a whirlwind of a morning and we had so much information to digest. My blood pressure was to be checked every two hours and blood was drawn every four to monitor the liver enzymes and platelet levels. Other than blood pressure medication that I took orally I was free of an IV or pain medication at this point - overall I felt fine. Early that evening my parents arrived and we had dinner while we waited for the doctors to update us on my latest lab work. It was actually "good" news my platelets hadn't dropped and had slightly increased - that meant that delivery was not necessary that evening, monitoring would continue and things would be reassessed in the morning. It was a slight relief that we still had time and we knew that every hour the baby was able to stay-put the better it was for development and decreased potential complication. Up to this point, I was told that c-section would be the only possibility for delivery but the doctor at this point noted I would potentially be able to deliver naturally, dependent on how things played out but it was a possibility. I was very happy to hear this - my hopes/ plans throughout my pregnancy was for a natural birth and so I clung to the hope that I would get to experience such a birth.
We decided that it was best for Matt to go home for the evening to take care of the dog and get some much needed sleep (which I'm sure he didn't get) - so I spent the night alone. I was lucky to have a private room, although I don't think I slept much, I shed many tears and was awoken often for blood pressure checks and blood work. However, I feel though that evening I came to terms with what was happening and felt that I could handle our situation - - I don't think we are given more than we are able to handle in life and felt that if this was the hand we were dealt than we had the capacity to handle it. I think Matt was far more scared than I was -- he was worried that he could potentially lose us both. For me, I didn't really put much consideration into the "thoughts" of loss - in my chosen field I have seen a lot, and worked with children who were preemies, many far more premature than we were dealing with and although some of them had challenges they had to overcome they were here - they made it. I knew the survival rate at 30 weeks looked good especially since she measured well on the fetal assessment and I believed we created a fighter who was meant to experience this world. Also, I felt that I (as well as Matt) was equipped with the knowledge and capacity to deal with the potential deficits and challenges that could potentially face us if complications led to a potential disability. Sure I hoped for best but also knew I was prepared for the worst-case scenario.
Tuesday, June 4
In the morning, we were visited by both the neonatologist and anesthesiologist to discuss potential outcomes and agree to certain course of treatments, when and if certain situations arose. The neonatologist confirmed what I already knew, that the survival outlook was good but had to inform us of the numerous complications that could occur. He explained the potential need for blood transfusions, ventilation, and other life saving interventions - we were well-informed, got the answers to the questions we had and felt in good hands. The meeting with the anesthesiologist was similar, although at this point I was hoping anesthesiologist wouldn't need to be part of my care plan but we had to be prepared for all outcomes. We were informed that "delivery" could happen one of two ways. One, I would go under local anesthetic for the c-section in which Matt would be allowed in the delivery room and I would be conscious. Two, I would need to be put under general anesthetic where I would be completely put out and Matt would not be able to be in the OR for the delivery. Of course, I was hoping that neither of these would need to be my option and that either induction or my body would naturally go into early labor - but of these two options we had hoped that local anesthetic could be the course of action. To this the anesthesiologist replied that in most cases they had seen this was not the route that had to be taken. It was then explained that it would depend on my platelet level at the time - if they were too low labor was not recommended due to the large amount of potential loss and local anesthetic would no longer be an option because of the potential of bleeding in the spinal cord that could lead to paralysis. My options were not looking good and at this point I was becoming a lot more scared about my overall outcome.
Other than those meetings the day was pretty uneventful, friends visited (bringing our first preemie outfits and a chance to talk about other things) - I was still feeling ok, the pain had yet to return and my labs were staying steady. I had received my second steroid injection which was an added bonus for baby but the doctor later explained that although it was helping baby it was actually helping masking how sick I was by causing a spike in my platelets levels - it was buying us more time but it was by no means "getting better". Monitoring would continue but the doctors believed it wasn't going to be much longer until we inevitably needed to take action.
Wednesday, June 5
Following the previous trend, I was awoken in the middle of the night around 2am and the pain had returned. I buzzed the nurses, they informed the doctors, and I immediately called Matt who was at home again to look after our pup. I was given pain medication, blood was drawn, and we were to wait for the labs to comeback for the doctor to make a decision on course of action. Around 6am we were informed I would have another fetal assessment around 11am in order to see how baby was. Seriously, I feel like we did a lot of waiting on tests and for appointments in this 3 day period, it was so hard "just to sit tight to see what the labs say", especially when we knew inevitably we would be dealing with the same outcome at some point.
Anyways at the fetal assessment it was found that the bloodflow to the baby was starting to become compromised and they felt that we needed to intervene as soon as possible. We again discussed the options, and I asked again if it were possible to induce labor to try for a vaginal delivery. The doctor said that they would check if my cervix had begun to soften at all...and it hadn't. We were told that at this point they didn't feel we had the time to attempt induction and that a c-section would be the fasted and best option.
Following the fetal assessment, wepatiently (ugh) waited to hear news on when we would be scheduled to prep for surgery - only to be told that we would need to be transferred to another hospital in the city as the current hospital NICU was at capacity. I was not happy about this - and later after talking with my obstetrician neither was she! She (as well as I) felt that the on-call OBGYN should have done all that they could to have kept my case at the hospital where all my previous consults had occurred - although the result would have been the same at least it would have been with people I had already met with - and as you will see I believe in a more timely fashion).
So again we waited, this time for the ambulance which came to transport me around 2pm, it was aquick, bumpy 15 minute ride in which my husband did not get to be with me as he drove our vehicle to the new hospital (to pay yet more and more money in parking..). He and my parents met us there and I was placed in a room to wait to be prepped for surgery which was "scheduled" for 4pm. Part of the prep was to start 2 IV's which took a gazillion 15 or so attempts to start, they actually had to call in the specialized IV team, I felt like a human pin-cushion at this point (and had the bruises to show it for weeks following this ordeal) and felt weaker, tired, and more faint every minute (my platelets were so low at this point and the IV was for a blood transfusion). So much so that I can't remember much of the prep, other than there being lots of nurses, more consults from specialist we had already met with at the previous hospital, and me spending the majority of the time trying to get my wedding rings off. I had started to swell even more and realized I still had my rings on (I'd been working on trying to get them off over the course of the past days) the nurses gave me lotions, we iced my finger for awhile, to no avail they wouldn't budge -- finally the nurse arrived with metal cutters and I sadly agreed to having them cut off (read: take off your rings early pregnant ladies!). Finally I was prepped and waiting (seeing the trend) for the doctor to be finished with an "emergency" (was I not an emergency?!) surgery. At this point, I felt the worst I had in days - and we just continued to wait and wait, finally around 5:45-6pm I was told they were ready, said goodbye to Matt (ensured we still agree on the name we had chosen as he would be the one to tell the name since I would be out) and my parents then was wheeled down the hall to the operating room. Transferred to the operating table, my arms strapped out to my side, there was yet another difficulty with IV or something regarding the anesthesia. From here again I just remember bright light, tonnes of nurses introducing themselves, questions, more talking, more waiting, and more poking. They kept saying the doctor was on the way, but it seemed like forever I'd been waiting, then at this point I was freezing and I began to shake, my teeth chattered, I couldn't focus on anything - blankets covered me yet I was still cold. I waited, waited, and then....darkness. I guess finally the doctor arrived.
Greta Elyse arrived at 7:01 via c-section 2lbs 9oz and 15 inches . My husband seen her immediately after she was examined. These were her first photos (our little fighter didn't even need to be intubated, just some oxygen, her strength amazed us, she still amazes us!)
After I "came to" from surgery, I was wheeled into the recovery room. Greta was there in an isolette, but sadly I vaguely remember. I do remember saying she's so small, asking is she ok, and wanting to touch her reaching out hitting plastic and not the soft warm newborn skin. It would be 2 days later that I would actually hold her in my arms on my chest. I wish that I had a better memory of the first moments of her life and I wish that I could recall these events better. But in the end, she arrived safely and healthy - just early and needed time to grow. Myself, I'm here too - I'm healthy. The few days after were rough - rougher than the days leading up to the birth, as I was on IV's, medications, and pain killers but that passed and I don't have any ongoing issues like some people who have experienced HELLP syndrome. We are both lucky. There are so many emotions attached to her birth. Part of me wishes they had taken action sooner and maybe I could have been induced, but all the time we took waiting - every extra minuted helped her strive and thrive, the latter is most important in the long run.
If you have any questions on my story, preterm birth or our NICU experience please feel free to contact me or comment below. I don't think anyone can ever be "prepared" for a preterm birth but if I can in anyway help with questions I'd be more than happy to answer them.
Have a great weekend!
I believe I was offered a wheelchair when we were transported to the fetal assessment, but I declined and walked to the fetal assessment (while writing this I asked my husband why I walked, and he says that I was so determined that I was not that ill), I think I should have set my pride aside and just went in wheelchair but anyways - we walked. We had an awesome ultrasound technician for the fetal assessment - she explained everything she was doing, told us what she was measuring and assured us that the baby was looking great. I did not have very good experience with ultrasound techs earlier in my pregnancy as I found them very cold and would never talk or explain anything - I get they can't say much as they aren't doctors but I always felt weird after previous ultrasounds! Her compassion and reassurance was really what we needed at this point! Following the fetal assessment I was admitted to the Antepartum unit to be monitored for the next 24-48 hours.
For the rest of the afternoon we rested, prepared questions for the doctors who we would be meeting with and just tried to put into perspective what was going on. It had been a whirlwind of a morning and we had so much information to digest. My blood pressure was to be checked every two hours and blood was drawn every four to monitor the liver enzymes and platelet levels. Other than blood pressure medication that I took orally I was free of an IV or pain medication at this point - overall I felt fine. Early that evening my parents arrived and we had dinner while we waited for the doctors to update us on my latest lab work. It was actually "good" news my platelets hadn't dropped and had slightly increased - that meant that delivery was not necessary that evening, monitoring would continue and things would be reassessed in the morning. It was a slight relief that we still had time and we knew that every hour the baby was able to stay-put the better it was for development and decreased potential complication. Up to this point, I was told that c-section would be the only possibility for delivery but the doctor at this point noted I would potentially be able to deliver naturally, dependent on how things played out but it was a possibility. I was very happy to hear this - my hopes/ plans throughout my pregnancy was for a natural birth and so I clung to the hope that I would get to experience such a birth.
We decided that it was best for Matt to go home for the evening to take care of the dog and get some much needed sleep (which I'm sure he didn't get) - so I spent the night alone. I was lucky to have a private room, although I don't think I slept much, I shed many tears and was awoken often for blood pressure checks and blood work. However, I feel though that evening I came to terms with what was happening and felt that I could handle our situation - - I don't think we are given more than we are able to handle in life and felt that if this was the hand we were dealt than we had the capacity to handle it. I think Matt was far more scared than I was -- he was worried that he could potentially lose us both. For me, I didn't really put much consideration into the "thoughts" of loss - in my chosen field I have seen a lot, and worked with children who were preemies, many far more premature than we were dealing with and although some of them had challenges they had to overcome they were here - they made it. I knew the survival rate at 30 weeks looked good especially since she measured well on the fetal assessment and I believed we created a fighter who was meant to experience this world. Also, I felt that I (as well as Matt) was equipped with the knowledge and capacity to deal with the potential deficits and challenges that could potentially face us if complications led to a potential disability. Sure I hoped for best but also knew I was prepared for the worst-case scenario.
Tuesday, June 4
In the morning, we were visited by both the neonatologist and anesthesiologist to discuss potential outcomes and agree to certain course of treatments, when and if certain situations arose. The neonatologist confirmed what I already knew, that the survival outlook was good but had to inform us of the numerous complications that could occur. He explained the potential need for blood transfusions, ventilation, and other life saving interventions - we were well-informed, got the answers to the questions we had and felt in good hands. The meeting with the anesthesiologist was similar, although at this point I was hoping anesthesiologist wouldn't need to be part of my care plan but we had to be prepared for all outcomes. We were informed that "delivery" could happen one of two ways. One, I would go under local anesthetic for the c-section in which Matt would be allowed in the delivery room and I would be conscious. Two, I would need to be put under general anesthetic where I would be completely put out and Matt would not be able to be in the OR for the delivery. Of course, I was hoping that neither of these would need to be my option and that either induction or my body would naturally go into early labor - but of these two options we had hoped that local anesthetic could be the course of action. To this the anesthesiologist replied that in most cases they had seen this was not the route that had to be taken. It was then explained that it would depend on my platelet level at the time - if they were too low labor was not recommended due to the large amount of potential loss and local anesthetic would no longer be an option because of the potential of bleeding in the spinal cord that could lead to paralysis. My options were not looking good and at this point I was becoming a lot more scared about my overall outcome.
Other than those meetings the day was pretty uneventful, friends visited (bringing our first preemie outfits and a chance to talk about other things) - I was still feeling ok, the pain had yet to return and my labs were staying steady. I had received my second steroid injection which was an added bonus for baby but the doctor later explained that although it was helping baby it was actually helping masking how sick I was by causing a spike in my platelets levels - it was buying us more time but it was by no means "getting better". Monitoring would continue but the doctors believed it wasn't going to be much longer until we inevitably needed to take action.
Wednesday, June 5
Following the previous trend, I was awoken in the middle of the night around 2am and the pain had returned. I buzzed the nurses, they informed the doctors, and I immediately called Matt who was at home again to look after our pup. I was given pain medication, blood was drawn, and we were to wait for the labs to comeback for the doctor to make a decision on course of action. Around 6am we were informed I would have another fetal assessment around 11am in order to see how baby was. Seriously, I feel like we did a lot of waiting on tests and for appointments in this 3 day period, it was so hard "just to sit tight to see what the labs say", especially when we knew inevitably we would be dealing with the same outcome at some point.
Anyways at the fetal assessment it was found that the bloodflow to the baby was starting to become compromised and they felt that we needed to intervene as soon as possible. We again discussed the options, and I asked again if it were possible to induce labor to try for a vaginal delivery. The doctor said that they would check if my cervix had begun to soften at all...and it hadn't. We were told that at this point they didn't feel we had the time to attempt induction and that a c-section would be the fasted and best option.
Following the fetal assessment, we
So again we waited, this time for the ambulance which came to transport me around 2pm, it was a
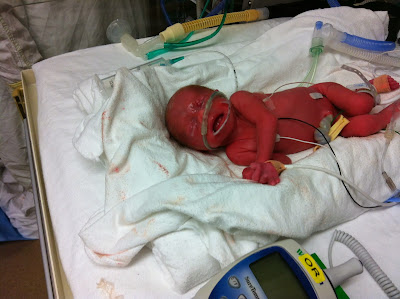
Greta Elyse arrived at 7:01 via c-section 2lbs 9oz and 15 inches . My husband seen her immediately after she was examined. These were her first photos (our little fighter didn't even need to be intubated, just some oxygen, her strength amazed us, she still amazes us!)
(to give you some perspective - in the top photo you can see a hand-held thermometer and it's big in perspective to her)
After I "came to" from surgery, I was wheeled into the recovery room. Greta was there in an isolette, but sadly I vaguely remember. I do remember saying she's so small, asking is she ok, and wanting to touch her reaching out hitting plastic and not the soft warm newborn skin. It would be 2 days later that I would actually hold her
If you have any questions on my story, preterm birth or our NICU experience please feel free to contact me or comment below. I don't think anyone can ever be "prepared" for a preterm birth but if I can in anyway help with questions I'd be more than happy to answer them.
Have a great weekend!





This is a lovely account. She was so itty bitty and precious. Lucky to have you for her mama.
ReplyDeleteThanks Andrea. Was hard recalling it all -- as parts of it I would like to forget. She was so tiny, to us we were so use to it but now when we pull out her preemie clothes or hats she wore when she was first born, we can't get over how small they are! She will probably dress her dolls in some of it in a few years.
DeleteSame here, we were used to him being tiny so it didn't seem so crazy to us. But now looking at those tony clothes or seeing pictures of us holding him it hits us how TINY TINY TINY he was. :-)
DeleteSuch a journey Greta has had already! Thanks for sharing.
ReplyDeleteyes it was quite the journey. thanks of reading!
DeleteWow, so much waiting! I didn't have to wait long because my platelets were super low and went even lower the 2nd time the did blood tests. I only had time for one steroid shot. We had the c-section approx 12 hours after I arrived at the hospital. Crazy! I like how you guys discussed the name! We hadn't even decided on one at the time so our boy went nameless for about 24hours before we made the final decision. :-P
ReplyDelete